Abstract
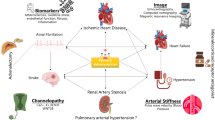
Primary aldosteronism (PA) is common, but usually overlooked in the elderly, old, and very old patients in whom the already high absolute risk of cardiovascular events, particularly atrial fibrillation, can be further increased by PA. Although in the last two decades there has been an explosion of studies devoted to diagnosis, subtyping, and treatment of PA, only relatively scant investigation has addressed these topics in patients older than 65 years of age. This narrative review fills a gap of information on the challenges of diagnosing and managing the PA patients who are 65 years old and older with particular attention to the benefit/risk ratio of pursuing the diagnosis in this cohort, which is markedly expanding owing to ageing of the population worldwide.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Hung C-S, Sung S-H, Liao C-W, Pan C-T, Chang C-C, Chen Z-W, et al. Aldosterone induces vascular damage—a wave reflection analysis study. Hypertension. 2019;74:623–9.
Rossi GP, Maiolino G. Excess arterial damage in hyperaldosteronism: further evidence from pressure wave analysis. Hypertension. 2019;74:502–4.
Monticone S, Burrello J, Tizzani D, Bertello C, Viola A, Buffolo F, et al. Prevalence and clinical manifestations of primary aldosteronism encountered in primary care practice. J Am Coll Cardiol. 2017;69:1811–20.
Käyser SC, Dekkers T, Groenewoud HJ, Van Der Wilt GJ, Carel Bakx J, Van Der Wel MC, et al. Study heterogeneity and estimation of prevalence of primary aldosteronism: a systematic review and meta-regression analysis. J Clin Endocrinol Metab. 2016;101:2826–35.
Baudrand R, Guarda FJ, Fardella C, Hundemer G, Brown J, Williams G, et al. Continuum of renin-independent aldosteronism in normotension. Hypertension. 2017;69:950–6.
Funder JWW, Carey RMM, Mantero F, Murad MHH, Reincke M, Shibata H, et al. The management of primary aldosteronism: case detection, diagnosis, and treatment: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2016;101:1889–916.
Rossi GP. Primary aldosteronism: JACC state-of-the-art review. J Am Coll Cardiol. 2019;74:2799–811.
Hiramatsu K, Yamada T, Yukimura Y, Komiya I, Ichikawa K, Ishihara M, et al. A screening test to identify aldosterone-producing adenoma by measuring plasma renin activity. Results in hypertensive patients. Arch Intern Med. 1981;141:1589–93.
Rossi GP, Seccia TM, Palumbo G, Belfiore A, Bernini G, for the Prevalence in hYpertension (PAPY) Study Investigators, et al. Within-patient reproducibility of the aldosterone:renin ratio in primary aldosteronism. Hypertension. 2010;55:83–9.
Maiolino G, Rossitto G, Bisogni V, Cesari M, Seccia TM, Plebani M, et al. Quantitative value of aldosterone-renin ratio for detection of aldosterone-producing adenoma: The Aldosterone-Renin Ratio for Primary Aldosteronism (AQUARR) study. J Am Heart Assoc. 2017;6:e005574.
Rossi GP, Ceolotto G, Rossitto G, Seccia TM, Maiolino G, Berton C, et al. Prospective validation of an automated chemiluminescence-based assay of renin and aldosterone for the work-up of arterial hypertension. Clin Chem Lab Med. 2016;54:1441–50.
Rossi GP, Bisogni V. An app for the diagnosis of primary aldosteronism. Am J Hypertens. 2016;29:660–1.
Nanba K, Vaidya A, Williams GH, Zheng I, Else T, Rainey WE. Age-related autonomous aldosteronism. Circulation. 2017;136:347–55.
Nakama C, Kamide K, Kawai T, Hongyo K, Ito N, Onishi M, et al. The influence of aging on the diagnosis of primary aldosteronism. Hypertens Res. 2014;37:1062–7.
Ma L, Song Y, Mei M, He W, Hu J, Cheng Q, et al. Age-related cutoffs of plasma aldosterone/renin concentration for primary aldosteronism screening. Int J Endocrinol. 2018;2018:article ID:8647026.
Luo Q, Li NF, Yao XG, Zhang DL, Abulikemu SFY, Chang GJ, et al. Potential effects of age on screening for primary aldosteronism. J Hum Hypertens. 2016;30:53–61.
Hannemann A, Friedrich N, Lüdemann J, Völzke H, Rettig R, Peters J, et al. Reference intervals for aldosterone, renin, and the aldosterone-to-renin ratio in the population-based study of health in pomerania (SHIP−1). Horm Metab Res. 2010;42:392–9.
Gan W, Lin W, Ouyang J, Li Y, Chen D, Yao Z, et al. High efficiency of the aldosterone-to-renin ratio in precisely detecting primary aldosteronism. J Hum Hypertens. 2019;33:57–61.
Staessen J, Amery AFR. Isolated systolic hypertension in the elderly. J Hypertens. 1990;8:393–405.
Strauch B, Petrak O, Zelinka T, Wichterle D, Holaj R, Kasalicky M, et al. Adrenalectomy improves arterial stiffness in primary aldosteronism. Am J Hypertens. 2008;21:1086–92.
Franklin SS, Gustin W 4th, Wong ND, Larson MG, Weber MA, Kannel WB, Levy D. Hemodynamic patterns of age-related changes in blood pressure. The Framingham Heart Study. Circulation. 1997;96:308–15.
Rossi GP, Seccia TM, Pessina AC. A diagnostic algorithm–the holy grail of primary aldosteronism. Nat Rev Endocrinol. 2011;7:697–9.
Seccia TM, Fassina A, Nussdorfer GG, Pessina AC, Rossi GP. Aldosterone-producing adrenocortical carcinoma: an unusual cause of Conn’s syndrome with an ominous clinical course. Endocr Relat Cancer. 2005;12:149–59.
Zhu L, Zhang Y, Zhang H, Zhou W, Shen Z, Zheng F, et al. Comparison between adrenal venous sampling and computed tomography in the diagnosis of primary aldosteronism and in the guidance of adrenalectomy. Medicine. 2016;95:1–6.
Takeda M, Yamamoto K, Akasaka H, Rakugi H, Naruse M, Takeda Y, et al. Clinical characteristics and postoperative outcomes of primary aldosteronism in the elderly. J Clin Endocrinol Metab. 2018;103:3620–9.
Rossi GP, Mulatero P, Satoh F. 10 good reasons why adrenal vein sampling is the preferred method for referring primary aldosteronism patients for adrenalectomy. J Hypertens. 2019;37:603–11.
Rossi GP, Barisa M, Allolio B, Auchus RJ, Amar L, Cohen D, et al. The Adrenal Vein Sampling International Study (AVIS) for identifying the major subtypes of primary aldosteronism. J Clin Endocrinol Metab. 2012;97:1606–14.
Akasaka H, Yamamoto K, Rakugi H, Nagasawa M, Nakamaru R, Ichijo T, et al. Sex difference in the association between subtype distribution and age at diagnosis in patients with primary aldosteronism. Hypertension 2019;74:368–74.
Iacobone M, Mantero F, Basso SM, Lumachi F, Favia G. Results and long-term follow-up after unilateral adrenalectomy for ACTH-independent hypercortisolism in a series of fifty patients. J Endocrinol Investig. 2005;28:327–32.
Vriens MR, WMCM Vorselaars, Nell S, Postma EL, Zarnegar R, Drake FT, et al. Clinical outcomes after unilateral adrenalectomy for primary aldosteronism. JAMA Surg. 2019;154:e185842.
Rossi GP, Rossitto G, Amar L, Azizi M, Riester A, Reincke M, et al. The clinical outcomes of 1625 patients with primary aldosteronism subtyped with adrenal vein sampling. Hypertension. 2019;74:800–8.
Liang KW, Jahangiri Y, Tsao TF, Tyan YS, Huang HH. Effectiveness of thermal ablation for aldosterone-producing adrenal adenoma: a systematic review and meta-analysis of clinical and biochemical parameters. J Vasc Interv Radiol. 2019;30:1335–42.e1.
Hokotate H, Inoue H, Baba Y, Tsuchimochi S, Nakajo M. Aldosteronomas: experience with superselective adrenal arterial embolization in 33 cases. Radiology. 2003;227:401–6.
Wada N, Shibayama Y, Umakoshi H, Ichijo T, Fujii Y, Kamemura K, et al. Hyperkalemia in both surgically and medically treated patients with primary aldosteronism. J Hum Hypertens. 2017;31:627–32.
Tahir A, McLaughlin K, Kline G. Severe hyperkalemia following adrenalectomy for aldosteronoma: prediction, pathogenesis and approach to clinical management- a case series. BMC Endocr Disord. 2016;16:43.
Hundemer GL, Baudrand R, Brown JM, Curhan G, Williams GH, Vaidya A. Renin phenotypes characterize vascular disease, autonomous aldosteronism, and mineralocorticoid receptor activity. J Clin Endocrinol Metab. 2017;102:1835–43.
Hundemer GL, Curhan GC, Yozamp N, Wang M, Vaidya A. Cardiometabolic outcomes and mortality in medically treated primary aldosteronism: a retrospective cohort study. Lancet Diabetes Endocrinol. 2018;6:51–9.
Capelli I, Gasperoni L, Ruggeri M, Donati G, Baraldi O, Sorrenti G, et al. New mineralocorticoid receptor antagonists: update on their use in chronic kidney disease and heart failure. J Nephrol. 2010;33:37–48.
Lim PO, Jung RT, MacDonald TM. Raised aldosterone to renin ratio predicts antihypertensive efficacy of spironolactone: a prospective cohort follow-up study. Br J Clin Pharmacol. 1999;48:756–60.
Dietz JD, Du S, Bolten CW, Payne MA, Xia C, Blinn JR, et al. A number of marketed dihydropyridine calcium channel blockers have mineralocorticoid receptor antagonist activity. Hypertension. 2008;51:742–8.
Acknowledgements
GPR research was mostly supported by research grants from the EU COST-ADMIRE BM1301 and ENSAT-HT 633983, FORICA (The Foundation for advanced Research In Hypertension and Cardiovascular diseases) and the Società Italiana dell’Ipertensione Arteriosa and The University of Padua.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cesari, M., Seccia, T.M., Maiolino, G. et al. Primary aldosteronism in elderly, old, and very old patients. J Hum Hypertens 34, 807–813 (2020). https://doi.org/10.1038/s41371-020-00395-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-020-00395-2