We present our experience of a wide variety of scrotal conditions using mainly ultrasound. MR was used in few cases for further assessment.
The processes are separated into non-tumoral and tumoral and include testicular and extratesticular conditions.
A) NON TUMORAL PATHOLOGY
TESTICULAR (Fig. 1, Fig. 2, Fig. 3, Fig. 4, Fig. 5)
1.1 CYSTIC LESIONS
Cystic or encapsulated fluid collections are relatively common benign lesions that may present as palpable testicular lumps.
Most cysts arise in the epididymis,
but they can be developed in all anatomical structures of the scrotum.
US diagnosis of simple cysts is based on the characteristic sonographic findings of these lesions (anechoic,
imperceptible wall,
avascular,
posterior wall thickening).
Sometimes testicular cyst contains echoic material: if the material is mobile,
the cyst is probably benign; if it is fixed,
malignant lesions must be discarded.
- Tunica albuginea cyst: The tunica albuginea is a fibrous sheath that contains the testicle.
Cysts in this location are easily palpable and they might be painful when they become larger.
At US examination,
a simple anechoic cyst together with signs of compression of the adjacent testicular parenchyma may be noted.
- Testicular cyst: These cysts are usually not palpable and incidentally found during US examination.
They arise in connection with focal dilatation of the seminiferous tubules due to malformation or as a result of inflammatory episode.
1.2 EPIDERMOID CYST
Epidermoid cyst are rare,
benign tumors with varied sonographic appearances secondary to the variability in maturation and quantity of keratin.
It usully presents in 20 to 40 years old men and can range from 1 to 3 cm in size.
Different sonographic appearances have been described but the classic onion rign appearance is considered characteristic,
which is seen as an onion ring configuration due to alternating layers of hypo and hyperechogenicity.
1.3 TESTICULAR SPERMATOCELE
An intratesticular spermatocele is a cystic intraparenchymal lesion attached to the mediastinum in the area of the rete testis.
It communicates with the seminiferous tubules,
unlike the simple ectasia of the rete testis,
which does not communicate directly.
The cysts contain spermatozoa and can be septated.
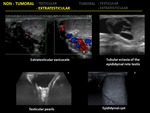
1.4 TUBULAR ECTASIA OF THE RETE TESTIS
Tubular ectasia of the rete testis is a benign condition resulting from partial or complete obliteration of the efferent ducts that cause ectasia of the rete testis.
It usually occurs in men over 55 years old and is frequently bilateral.
Findings of cystic dilatations adjacent to the mediastinum testis and the presence of epididymal cysts are charecteristics of tubular ectasia.
US findings can differ depending on the progress of the dilatation.
It can be limited to a few dilated tubules near the testicular hilum o appear as a network of small cysts occupying the central portion of the testicle.
Although ectasia of the rete testis is a benign condition,
it may cause olygospermia and azoospermia and consequent infertility.
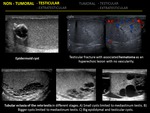
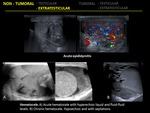
1.5 HEMATOMA
Testicular hematomas are commonly seen secondary to trauma or testicular biopsy.
US findings depend on the age of the hematoma; acute hematomas appear hyperechoic and subsequently become complex with cystic components.
They are avascular on color US Dopper.
1.6 LEYDIG CELL HYPERPLASIA
Testicular Leydig cell hiperplasia is a rare benign condition that is characterized by small (1-6mm),
multifocal,
and frequently bilateral testicular nodules.
In the primary form,
male children may present with precocious puberty,
whereas in the secondary form,
that usually occurs in adults,
these nodules are usually not palpable and the diagnosis is made as an incidental finding.
In contrast,
patients with Leydig´s cell tumor present with endocrine abnormalities such as adult feminization,
gynecomastia and decreased libido.
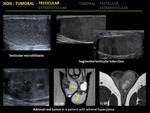
1.7 TESTICULAR MICROLITHIASIS
Testicular microlithiasis (TM) is an uncommon condition usually found incidentally at US.
It is characterized by intratubular calcifications within a multilayered envelope cointaining organelles,
vesicles and collagen fibers.
This fibrous envelope is presumed to be responsible for the absence of acoustic shadowing of the calcifications in ultrasound,
although it could be also attributable to small size of the foci.
Its typical US appearance is multiple nonshadowing echogenic foci measuring 2-3mm and randomly scattered throughout the testicular parenchyma.
The presence of 5 or more foci per transducer field in one testis is suggestive of TM.
It has been believed for years that TM could lead to testicular cancer but it has not been confirmed and,
nowadays,
the presence of TM alone in absence of other risk factors is not an indication for further study.
1.8 ADRENAL REST TUMOR
Congenital testicular adrenal rests are seen in about 29% of patients with congenital adrenal hiperplasia (CAH).
CAH is an autosomas recessive disease characterized by a deficiency of adrenocortical enzymes.
An increase of adrenocorticotropic hormone (ACTH) levels causes hiperplasia of adrenal remnants in the testes in patients with CAH and results in development of intratesticular masses,
that typically regress with treatment.
Sonographically,
the masses appear as hypoechoic intratesticular masses in both testes typically located in the region of mediastinum testis. US is the modality of choice for their diagnosis,
however,
MRI can also assist as a problem-solving tool in some cases.
Testicular adrenal rests appear isointense on T1 and hypointense on T2 weighted images with a diffuse enhancement pattern after gadolinium administration.
1.9 SEGMENTAL TESTICULAR INFARCTION
Focal or segmental testicular infarct usually occurs in the third decade of life and patients may present with an acute scrotum.
It is most commonly idiopathic in origin but may also occur secondary to other etiologies such as acute epididymo-orchitis,
which can cause obstruction of the adjacent testicular blood supply.
The ultrasound appearance of a segmental infarct is that of a focal mixed echogenic or hypoechoic lesion with wedge shape that sometimes may simulate a testicular tumor.
Color flow Doppler examination demonstrate absent vascularity within the affected region,
thus distinguishing it from a tumor.
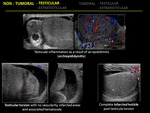
1.10 ORCHITIS
Primary orchitis in isolation is rare and most commonly caused by mumps.
Bilateral involvement is seen in 14%-35% of the cases.
At US,
the affected testes appear enlarged with decreased echogenicity.
Because intratesticular venous flow is difficult to detect in normal testes,
increased and easily detected venous flow is highly suggestive of orchitis.
1.11 TESTICULAR TORSION
US is considered the first step in evaluation of this condition and plays an important role in helping differantiate acute epididymo-orchitis from testicular torsión,
which is a surgical emergency.
Both manifest with acute pain and swelling and clinical differentiation may be difficult.
Testicular torsion can occur at any age; however,
it is most frequent is adolescent boys Two types of torsion have been described: extravaginal and intravaginal.
Extravaginal torsion occurs exclusively in newborns and it takes place outside the tunica vaginalis when the testes are not fixed and are free to rotate.
The affected neonate presents iwth swelling,
discoloration of the scrotum of the affected side and a firm painless mass in the scrotum.
US color Doppler show no flow in the testis or spermatic cord.
Intravaginal torsion occurs within the tunica vaginalis.
The predisposing factors include a long and narrow mesentery in which the tunica vaginalis completely encircles the epididymis,
distal spermatic cord and testis rather than attaches to the posterior aspect of the testis.
The deformity leaves the testis free to move and rotate within the tunica vaginalis.
Patients with acute torsion present after a sudden onset of pain followed by nausea,
vomiting and a low-grade fever.
Physical examination reveals a swollen,
tender and inflammed hemiscrotum.
The cremasteric réflex is usually absent and the pain cannot be relieved by elevating the scrotum.
In testicular torsion,
venous obstruction occurs first,
followed by obstruction of arterial flow and ultimately by testicular ischemia.
US findings vary with the duration and degree of rotation of the spermatic cord.
Gray-scale images are nonspecific for testicular torsion and often appear normal if the torsion has just occurred.
Testicular swelling and decreased echogenicity are the most commonly enoutered findings 4-6 hours after the onset of torsion.
At 24 hours after the onset,
the testis has a hetergeneous echotexture secondary to vascular congestion,
hemmorrhage and infarction.
In the setting of testicular torsion,
normal testicular echogenicity is a strong predictor of testicular viability. Because gray-scale US findings are often normal in the early phases of torsion,
the Doppler component of the examination is essential.
The absence of testicular flow at color and power Doppler US is considered diagnostic of ischemia.
1.12 TESTICULAR APPENDIX TORSION
Normal appendix testis appear as a small ovoid structure,
usually at the upper pole of the testis,
and better seen by the presence of fluid around the testis.
Patients with torsion of the appendix testis and appendix epididymis present with acut scrotal pain,
but there are usually no other physical symptoms and the cremasteric réflex can still be stimulated.
The classic finding al physical examination is a small firm nodule that is palpable on the superior aspect of the testis and exhibits bluish discoloration through the overlying skin (so called the blue dot sign).
Approximately 91-95% of twisted testicular appendices involve the appendix testis and occur most often in boys of 7-14 years old.
The pain usually resolves in 2-3 days,
with atrophy of the appendix.
This atrophied appendix may calcify and fall to the scrotal burse,
forming free rounded calcifications called scrotal pearls.
US evaluation of torsion usually reveals a hyperechoic mass with a central hypoechoic area adjacent to the testis or epididymis.
Reactive hidrocele and skin thickening are common findings.
Increased peripheral flow can be seen around the twisted appendage.
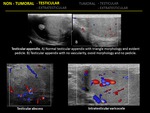
1.13 TESTICULAR ABSCESS
An intratesticular abscess most frequently results from epididymo-orquitis and less commonly from a superadded infection in post-traumatic testicular hematomas or testicular infarcts.
These patients present with an acute scrotum and high fever.
Ultrasonography is imaging modality of choice and demonstrates a hypoechoic lesion within the testis with low-level echoes and shaggy margins.
Color flow Doppler US show absent internal vascularity with increased peripheral hyperemia.
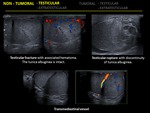
1.14 TESTICULAR INJURIES
- Fracture: A testicular fracture appears on US examination as a linear echogenic band that extends across the testicular parechyma and represents a break in the normal testicular architecture.
The overall contours remains smooth,
as the testicular shape and tunica albuginea are mantained.
Associated hematoma or hematocele may be seen.
Doppler imaging determines vascular integrity; If flow is absent,
emergency surgery is indicated as it represents testicular ischemia.
- Rupture: There is hemorrhage and extrusión os testicular contents into the scrotal sac.
Discontinuity of the echogenic tunica albuginea in indicative of testicular ruptura and needs emergency surgery. US demonstrates poorly defined testicular margins and heterogeneous echotexture with focal hyperechoic or hypoechoic areas in the testicular parenchyma corresponding to areas of hemorrhage or infarction.
Associated hematocele or wall thickening may be seen.
Color flow Doppler shows decreced flow or no flow.
1.15 INTRATESTICULAR VARICOCELE
Intratesticular varicocele is a rare entity reported in fewer than 2% of symptomatic men undergoing testicular sonography as opposed to extratesticular varicocele,
which are present in 15% - 20% of men.
Patients with intratesticular varicocele may have testicular pain due to venous congestion,
resulting in streching of the tunica albuginea.
Intratesticular varicoceles are usually associated with extratesticular varicoceles and their location may be subcapsular or adjacent to mediastinum testis.
Gray-scale sonography demonstrate tubular or serpertine structures more than 2mm in diameter with a positive Valsalva maneuver in color flow Doppler,
confirming the venous origin.
Intratesticular varicoceles adjacent to the mediastinum testis may mimic tubular ectasia; however,
color flow Doppler helps to differentiate between the two.
1.16 TRANSMEDIASTINAL VESSEL
From the posterior aspect of the testis,
the tunica albuginea invaginates within the testis to form an incomplete septum called the mediastinum testis.
Sonographically,
it appears as an echogenic band of variable thickness that extends across the testis in the longitudinal axis.
Branches from the capsular artery of the testis carry blood toward the mediastinum and divide to form a network that carries blood into the testis.
As many as in one half of the normal testis,
a transmediastinal branch of the testicular artery crosses through the mediastinum to supply capsular arteries and is usually accompained by a large vein.
Ay US examination,
a linear hypoechoic band is observed in longitudinal axis that will reveal flow through it when using color flow Doppler.
1.17 GRANULOMATOUS DISEASES
- Sarcoidosis: It is a multisystemic chronic granulomatous disease that presents with pulmonary manifestations in about 75% of cases.
Patients with testicular sarcoidosis are usually asymptomatic and may present with a painless mass.
Sonographically,
sarcoid granulomas appear as single or multiple hypoechoic nodules within the testes and epididymis mimicking testicular tumors.
Although differentiating both of them may be difficult,
the presence of multiple bilateral lesions in conjuction with other systemic presentations should rise the suspicion of sarcoidosis.
- Wegener´s granulomatosis (WG): It is a type of necrotising vasculitis that mainly affects the respiratory tract,
paranasal sinuses and kidneys.
Urogenital involvement is rare,
mainly affecting the prostate gland.
Testicular involvement is exceptional,
but sometimes can as an isolated manifestation.
Ultrasounds findings include unilateral or bilateral masses with hypoechoic densities that may disappear after treatment with imunosupressants and steroids.
EXTRATESTICULAR (Fig. 6, Fig. 7, Fig. 8)
2.1 ACUTE AND CHRONIC EPIDIDYMITIS
- Acute epididymitis: It is a common cause of acute scrotal pain in adolescent boys and young adults.
In adolescents,
many instances are secondary to sexually transmitted organisms such as Chlamydia trachomatis and Neisseria gonorrhoeae.
In prepuberal boys and adults over 35 years of age,
the disease is most frequently caused by E.
Coli and Proteus mirabilis.
Complications of acute epididymits include orchitis due to direct spread of infection,
chronic pain,
infarction,
abscess,
gangrene,
infertility,
atrophy and pyocele. At clinical examination,
the scrotal pain can be relieved by elevating the scrotum (positive Pehn sign). Us findings consist in an enlarged and hyperemic hypoechoic or hyperechoic (presumably secondary to hemorrhage) epididymis and indirect signs of inflammation,
such as reactive hydrocele or pyocele with scrotal wall thickening.
- Chronic epididimitis: This condition is characterized by persistent pain in scrotal area. At US examination,
it is characterized by an enlarged epididymis and increased echogenicity.
There may be calcifications.
- Sperm granuloma: Also called epididymitis nodosa,
a type of chronic epididymitis,
occurs secondary to inflammation,
trauma and vasectomy.
Sperm granuloma is a granulomatous reaction to extravasated sperm cells and occurs after vasectomy in up to 40% of patients,
but only 3% of them present with pain. At US examination,
they appear as a well-defined hypoechoic intraepidiymal lesion.
Cystic changes of the epididymis and heterogenous echegenicity may be associated.
2.2 HYDROCELE
The normal scrotum contains a few milimiters of serous fluid between the layers of the tunica vaginalis.
A hidrocele is an abnormally large collection of serous fluid and is the most common cause of painless scrotal swelling.
A hidrocele may be idiopathic or may develop after trauma,
infection,
torsion or tumor.
At US they are anechoic fluid collections surrounding the testicle that sometimes can have low-echos due to proteinaceous material.
2.3 HEMATOCELE
It is an accumulation of blood within the tunica vaginalis and usually occurs after trauma or surgery.
Its US appearance varies according to the age of the hematoma.
In the acute phase,
it appears as an echoic fluid collection with fluid-fluid levels or internal echoes due to breakdown products or hemoglobin.
This becomes hypoechoic over time and a complex cystic collection with septations may be formed.
2.4 PYOCELE
A pyocele results from untreated epididymo-orchitis or rupture of an intratesticular abscess into the space between the layers of the tunica vaginalis.
Pyocele at US examination appears as complex cystic lesion with internal septations and loculations.
2.5 VARICOCELE
Idiopathic varicoceles are present in approximately 15% of adult men.
It is an abnormal dilatation of the veins of the spermatic cord and is usually caused by incompetent valves in the internal spermatic vein.
This results in impaired drainage of blood into the spermatic cord veins when the patients assumes an upright position or during a Valsalva maneuver.
It is more frequent in the left side and palpation reveals a scrotal mass that may feel like a bag of worms.
Non compressible varicoceles prompt evaluation of the retroperitoneum because it may be associated with left renal vein thrombus,
tumoral extension or retroperitoneal mass compressing left renal or testicular vein.
Diagnosis of varicocele is important because it may be associated with infertility and its treatment improves sperm quality in as many as 53% of the cases.
The US appearance of varicocele consists of multiple,
hypoechoic,
serpiginous tubular structures of varying sizes larger than 2mm in diameter.
Color flow Doppler will demonstrate retrograde filling during a Valsalva maneuver.
2.6 SCROTAL PEARLS
Scroliths or scrotal pearls are benign extratesticular macrocalcifications within the scrotum.
They are usually of no clinical significance.
Possible etiologies include microtrauma to scrotal region or prior torsion of a testicular appendix.
At US,
they hyperechoic extratesticular calcification with posterior acoustic shadow.
They may be floating freely if there is an accompanying hydrocele.
2.7 SCROTAL HERNIA
Clinical history and physical examination may be sufficient to enable diagnosis os an intrascrotal hernia.
US is helpful in patients with equivocal physical findings and in those presenting with acute inguinoscrotal swelling.
The hernial sac most commonly contains bowel or omentum.
Other rare contents include Meckel diverticulum and urinary bladder.
Gray scale US findings include a fluid or gas filled loop of bowel in the scrotum or hyperechoic mass in case omental fat is herniated.
2.8 FIBROUS PSEUDOTUMOR
A fibrous pseudotumor is a painless tumor of the tunica that clinically mimics testicular and paratesticular neoplasms.
Most of them arise from the tunica vaginalis.
It is a benign fibroinflammatory reaction that results in the formation of one or more nodules and diffuse thickening of the testicular capsule.
They are usually associated with hydrocele,
history of trauma or infection.
It may appear as a well-defined hyperechoic or hypoechoic mass on ultrasound depending from the tunica layers.
2.9 CYSTIC LESIONS
- Spermatoceles: Spermatocele represent cystic dilatation of tubules of the efferent ductules in the head of the epididymis.
They are usually unilocular but can be multilocular and may be associated with a prior vasectomy.
At US examination,
they are well defined hypoechoic lesions of 1-2 cm with posterior acoustic enhancement and often contein low level echogenic proteinaceous fluid and spermatozoa.
- Cyst of the epididymis: Epididymal cyst are less common than spermatoceles and may arise throughout the epididymis,
while spermatoceles almost always arise in the epididymal head.
At US examination are indistinguishable but usually epididymal cysts contain clear serous fluid.
- Cyst of the appendix testis and appendix epididymis: The appendices of the testis and epididymis are residual cells from the duct of Muller and they are commonly seen on US examinations.
They are clinically insignificant but may undergo torsion causing intense pain.
Cystic lesions of the appendix are uncommon.
2.10 UNDESCENDENT TESTIS
The differencial diagnosis nonpalpable testicle includes a congenitally absent testicle,
cryptorchid,
retractile,
atrophia,
or ectopic testicle.
The undescendent testis may be positioned anywhere along the normal path of descent.
The most common location is in the inguinal canal (72%),
followed by prescrotal (20%) and abdominal (8%) location.
At US examination,
the undescendent testis may be smaller and less echogenic than the normal testis.
2.11 POLYORCHIDISM
Polyorchidism or supernumerary testes is defined as the presence of more than two testes and is a very rare congenital anomaly.
They are usually located in the scrotum or less commonly in the inguinal canal or abdominal cavity.
Ultrasound shows normal echogenicity of the testes and the supernumerary testes are usually seen as a small solid nodule which is isoechoic to the testes and located lower than the normal ones.
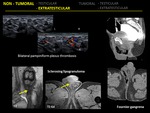
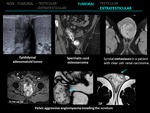
2.12 PAMPINIFORM VENOUS PLEXUS THROMBOSIS
Varicocele is a relatively common condition caused by the dilatation of the pampiniform plexus of the spermatic veins.
Spontaneus thrombosis of a varicocele is a rare event and difficult to diagnose as the patients present with an acute scrotum.
Ultrasonographic examination demonstrates pampiniform vein augmented in size and occupied by an echoic material.
Color Doppler US show no flow in the veins after Valsalva maneuvers.
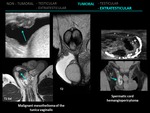
2.13 SCLEROSING LIPOGRANULOMA
Sclerosing lipogranulomas can be primary or secondary to a foreign body reaction.
Patients most often present with a painless intrascrotal mass that gradually increases in size.
Microscopic analysis shows lipid vacuoles surrounded by densely sclerotic stroma.
It has a high prevalence of spontaneous resolution and should be treated conservatively.
US demonstrates a hypoechoic extratesticular mass.
T1 and T2 weighted MR images typically show an enlarged heterogeneous mass that contains intravoxel fat in the upper scrotum or penoscrotal junction.
Heterogeneous enhancement is seen at contrast-enhanced imaging.
2.14 FOURNIER GANGRENE
Fournier gangrene is a polymicrobial necrotizing fascitis of the scrotumthat frequently extends to the lower abdominal wall.
The most common pathogens isolated in patients with this syndrome are Klebsiella,
Proteus,
Streptococcus,
Staphylococcus,
Peptostreptococcus,
Escherichia Coli and Clostridium perfringens.
Fournier gangrene constitutes a urologic emergency for which early recognition is demanded because of its high mortality rate.
The diagnosis is based primarily on physical examination,
however,
when clinical findings are ambiguous diagnostic imaging is useful.
Subcutaneous gas within the scrotal wall is the US hallmark of Founier gangrene.
Gas at US will appear as numerous hyperechoic foci with reverberation artifacts.
Other US findings include scrotal wall thickening with normal testicle and epididymis.
2.15 ACUTE IDIOPATHIC SCROTAL EDEMA
It is a benign,
self-limiting condition which is a rare cause of acute scrotal erythema.
Although it is more common in pediatric population,
it may be seen in adults.
It is a difficult but important diagnosis as it can avoid unnecessary surgical exploration.
Ultrasound examination may show bilateral scrotal skin thickening and hydrocele with increased vascularity on color Doppler US.
Normal appearance of the testes help diagnosis.
B) TUMORAL PATHOLOGY
TESTICULAR (Fig. 9, Fig. 10)
3.1 GERM CELL TUMOR
90% - 95% of testicular tumors are derived from germ cells.
They are divided in two groups: seminomatous and nonseminomatous.
- SEMINOMATOUS TUMORS: Seminomas are the most common type of testicular tumor and account for approximately 50% of all germ cell tumors.
They occur most in men aged in their 40s and are associated with the best prognosis because of their high sensitivity to radiation and chemotherapy.
They characteristically elevate β-human chorionic gonadotrophic hormone and α-fetoprotein level is never elevated in patients with pure seminoma.
Lymphatic spread to retroperitoneal lymph nodes and hematogenous metastases to lung and brain are seen in about 25% of patients at the time of presentation.
On gray-scale US,
seminoma appears as a homogeneous hypoechoic lesion and the entire testis is replaced by tumor in more than half cases.
They are usually confined by the tunica albuginea and rarely extend to peritesticular structures,
so they are conserved.
- NONSEMINOMATOUS TUMORS: Occurring most often in men aged in their 30s,
nonseminomatous tumors have multiple histologic patterns in 40% - 60% of cases.
The US appearance of tumors with a multihistologic pattern depend on the proportions of each component.
They often have an heterogeneous echotexture,
ill-defined margins,
echogenic foci and cystic components.
Approximately 60% of nonseminomatous tumors manifest with advanced disease.
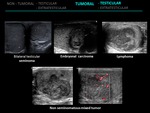
- Embryonal carcinoma: It is more aggressive than seminomas.
Most of them are mixed tumors.
Tumor invasion of the tunica albuginea is common and may distort the contour of the testis.
- Yolk sac tumor: These neoplasms occur most often in children younger than years and produce exclusively α-fetoprotein.
- Choriocarcinoma: It is a high malignancy tumor and elevates β-human chorionic gonadotrophic hormone levels.
Microscopic vascular invasion is common and explains the tendency of this tumor for early hematogenous metastasis,
specially to lungs.
- Teratoma: Teratomas are composed of all three germ cell layers; endoderm,
mesoderm and ectoderm.
They tend to be large and heterogeneous with calcifications and cystic components.
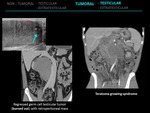
3.2 REGRESSED GERM CELL TUMOR (BURNED OUT)
It is usually a teratocarcinoma or a choriocarcinoma.
Occurs secondary to rapid tumor growth and results in the tumor outstripping its blood supply and in subsequent tumor regression.
Histologic examination reveals no tumoral cells,
only fibrosis and scar tissue.
It metastasizes and then burns out,
leaving metastases in the retroperitoneum.
They are often found at US while one is searching for a primary source of a retroperitoneal mass.
3.3 TERATOMA GROWING SYNDROME
This is a rare condition among patients with nonseminomatous germ cell tumors who present with enlarging metastatic abdominal masses despite appropiate systemic chemotherapy and normalized serum markers.
Histology of those resected lesions reveal benign mature teratomatous elements with no components of viable germ cell tumor.
3.4 NON-GERM CELL TUMOR
The majority of non germ cell tumors are sex cord-stromal tumors and include Leydig cell tumor and Sertoli cell tumor among others.
They are typically small and are usually discovered incidentally.
They do not have any specific US appearance but appear as well-definded hypoechoic lesions.
3.5 LYMPHOMA AND LEUKEMIA
- Lymphoma: In meno ver 60 years,
lymphoma is the most common testicular neoplasm and accounts for 50% of the cases.
Patients commonly present with enlarged testis.
Asynchronous involvement of the contralateral testis is more frequent that in other testicular tumors. At US,
homogeneously hypoechoic testes or multifocal hypoechoic lesions of various sizes.
Striated hypoechoic bands with parallel hyperechoic lines radiating peripherally from the mediastinum testis have also been described.
Color Doppler shows increased vascularity.
- Leukemia: Leukemic infiltration to the testis is not uncommon.
A blood-testis barrier limiting the effect of chemotherapeutic agents in the testes explains the persistence of leukemic cells in the testes after remission.
Thus,
any patient with a testicular mass found during the course of leukemia should undergo further study. The US appearance is similar to that of lymphoma.
3.6 LIPOMA
Intratestiular lipomas are rare benign fat-containing tumors.
They can appear isolated or as a testicular lipomatosis associated to Cowden´s syndrome (multiple hamartoma syndrome).
At US,
they appear as homogeneous hyperechoic nonshadowing lesions without flow at color Doppler imaging.
EXTRATESTICULAR (Fig. 11, Fig. 12)
4.1 ADENOMATOID TUMOR
Adenomatoid tumors constitute 30% of the rare paratesticular tumors.
The majority of them involve the epididymis and are accidentally found at physical examination.
It is a benign neoplasm characterized as a painless firm scrotal mass and with no reported metastases or recurrence after excision.
Ultrasound findings are inespecific as the appearence varies from hypoechoic to hyperchoic to isoechoic mass.
MRI can be performed as a complimentary tool for the diagnosis.
4.2 EPIDIDYMAL CYSTOADENOMA
Papillary cystoadenoma of the epididymis is a rare benign tumor often associated with Von Hipple Lindau disease.
It is clinically insignificant causing no discomfort.
The US appearance ranges from a primary cystic mass with an intramural solid component to an almost solid mass.
4.3 EXTRATESTICULAR LIPOMA
Lipoma is a benign mesenchymal tumor typically well defined and homogeneous at US and do not have internal flow on color Doppler images. MRI might be useful for confirmation,
as they show homogeneous high signal intensity on T1 and T2 weighted images and do no enhance with contrast.
Fat suppresion or in-phase and out-of-phase imaging can help distinguish between lipoma and hematoma or proteinaceous cyst.
4.4 SPERMATIC CORD SARCOMA
Sarcoma is the most frequent malignant tumor of the spermatic cord.
It usually tends to occur in older individuals and manifests as large complex solid masses.
In general,
sarcomas are heterogeneous masses with increased vascularity in US and avid enhancement in MRI.
4.5 METASTASES
Scrotum metastases are uncommon and usually occur in patients with a known malignancy in an advanced stage.
The most common primary tumors are prostate,
lung,
melanoma,
colon and kidney tumors.
4.6 MALIGNANT MESOTHELIOMA OF THE TUNICA VAGINALIS
This is an extremely rare tumor that develops from the mesothelial cells of the tunica vaginalis.
Malignant mesothelioma should be included in the differential diagnosis of a rapidly growing hydrocele.
US findings include hydrocele and wall thickening and,
less frequently,
a slightly hypoechoic mass attached to the parietal layer of the tunica.
T1 and T2 weighted MRI may show iso to slightly hyperintense masses and contrast enhancement is usually present when using Gadolinio.